What is sinus surgery anyway? Sinus surgery is surgical treatment to ventilate the obstructed air pockets within the facial bones. This includes the cheek sinuses, the forehead sinuses, the sinuses between the eyes and a sinus behind the eyes. Sinus surgery has gone through many evolutions over the past 50 years. Before nasal endoscopes and good lighting systems, surgery was done with skin incisions directly over the sinuses infected. This was done also with very poor CT scan information. In the late 1980s we began to see small nasal endoscopes being used for sinus surgery through the nostrils. This greatly reduced the need for cutting through skin, but it took a while for surgeons to become trained in good comprehensive surgery with endoscopes. We went through phases, first maximally reductive phase where we would remove as much sinus tissue as possible to try to comprehensively cure infection. We realized after several years that this was too aggressive and often created more problems than it solved. Endoscopic sinus surgery became less and less aggressive, focusing instead on preserving normal healthy anatomy and creating ventilation channels that allowed our own body’s immune system to work better. The next major shift came about around 2005. A much less aggressive sinus dilation procedure was invented. This allowed for small balloons to dilate the natural sinus openings for the frontal, maxillary, and sphenoid sinuses. In this case we were not removing any tissue but simply improving sinus ventilation. This has rapidly replaced about 50% of sinus surgery nationwide. We find that many people benefit greatly from this. As an added bonus the side effects, risks and recovery to this “surgery” are much less. These balloon sinuplasty procedures are now able to be done in the office under local anesthesia and minimal sedation. Typically simple over-the-counter medications are used to treat pain and discomfort for 24 hours.
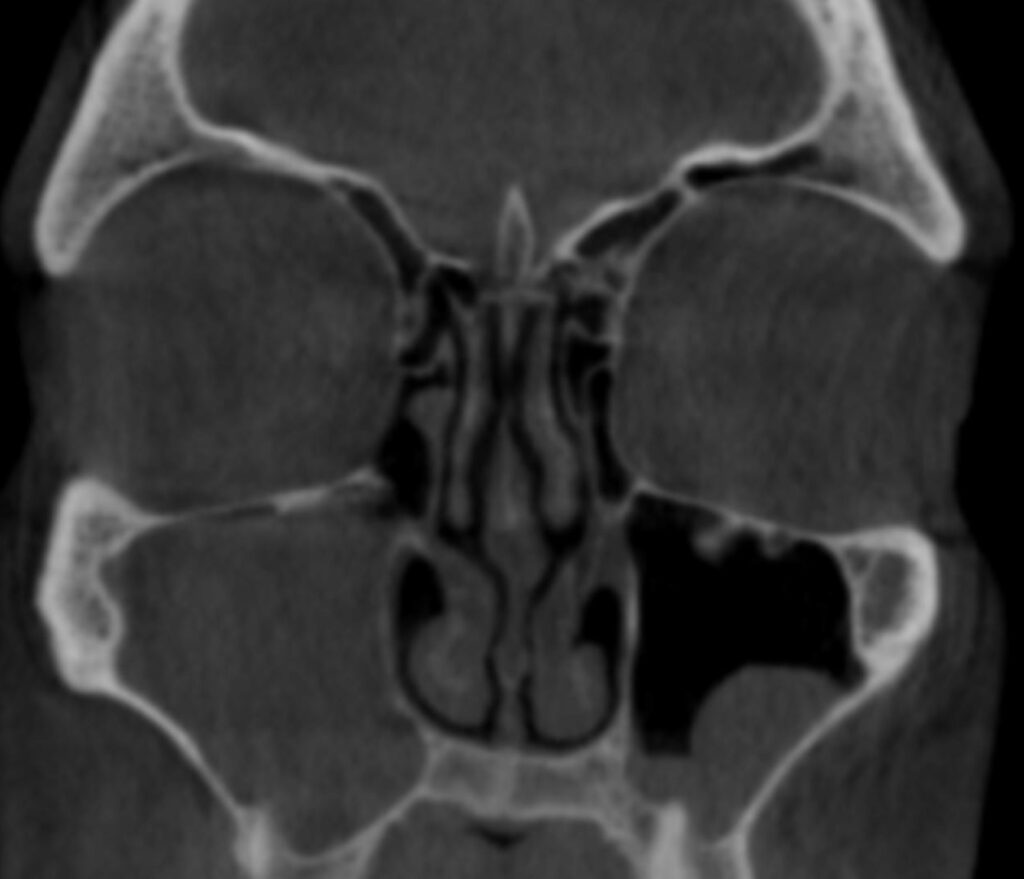
What If I am offered endoscopic sinus surgery? Most of us believe that endoscopic sinus surgery is much more important if there are coexisting nasal polyps, sinus masses, or more severe infection. It is also more useful if there is scarring of sinus openings from prior surgery. In patients with more severe disease on CT scan, more aggressive bacterial infections, or have lesions that need to have a good biopsy I am more likely to recommend endoscopic sinus surgery in the operating room. Surgery in the operating room allows us to do more cutting and removal of tissue when needed. Recovery is not severe, but is considerable for several days. However with severe disease, polyps, or masses is basically necessary I think. Usually before considering any sinus procedure we will have treated several weeks with antibiotics, attempted to get bacterial cultures, and have done nasal endoscopy. The sinus CT scan serves as our roadmap for surgery, both deciding if surgery is necessary and deciding the extent of surgery necessary.
For milder disease on sinus CT imaging, and patients without masses or severe scarring, office based minimal procedures such as the balloon sinuplasty is more favorable. The recovery is quick, hardly missing any work and hardly having any downtime. Furthermore, it subscribes to the theory that less is more, while preserving as much normal tissue as possible we are creating sizable ventilation channels into the sinuses to allow your body’s natural immunity every opportunity to restore health.
What is even better, we actually have pretty good long-term data showing the effectiveness of these balloon procedures on long-term sinus recovery.
In short, the more severe nasal blockage is, the more severe the sinus infection is on CT scanning tends to favor endoscopic sinus surgery in the operating room. Less severe sinus disease tends to respond better to the office procedures such as balloon sinuplasty.