Parathyroid Surgery

If you find yourself reading this page and researching parathyroid disease, you have likely been diagnosed with primary hyperparathyroidism, the most common disease of the parathyroid glands. Most people live their whole lives without knowing what a parathyroid gland does or what can go wrong with them, but parathyroid glands serve a very important role in the maintenance of the body’s calcium levels. Fortunately, primary hyperparathyroidism is a benign disease which can be cured with surgical removal of the affected gland or glands through an operation called a parathyroidectomy.
The parathyroid glands regulate the body’s calcium level through the production of parathyroid hormone (PTH). The parathyroid glands are located deep at the base of the neck near the thyroid gland, and each person has a total of four glands. Each side of the neck has an upper parathyroid gland located deeper in the neck near the nerve that activates the vocal cord (recurrent laryngeal nerve) and a lower gland located closer to the surface of the skin on the bottom portion of the thyroid. The exact locations of these glands may vary, particularly the lower glands which can sometimes even be found very deep inside the chest. Fortunately, this is relatively rare and the glands are found in predictable anatomic locations. Parathyroid glands can develop a benign growth called an adenoma which produces too much PTH and causes a condition called primary hyperparathyroidism. The first sign of this condition is an elevated blood calcium level, but hyperparathyroidism can lead to kidney stones, osteoporosis, depression, and bone pain. In many instances, the disease is present for months to years before it is diagnosed. Symptoms which are at times somewhat vague can be difficult to notice as they progress slowly over time.
The diagnosis of hyperparathyroidism is made through blood work alone. Imaging studies such as ultrasound and sestamibi scanning (nuclear medicine test) are only used to assist with surgical planning. Parathyroid surgery is tricky because neither the degree of calcium elevation nor the size of the abnormal gland or glands correlates with the disease severity. Larger adenomas are easier to identify before surgery with imaging studies, but with parathyroid adenomas, size doesn’t matter.
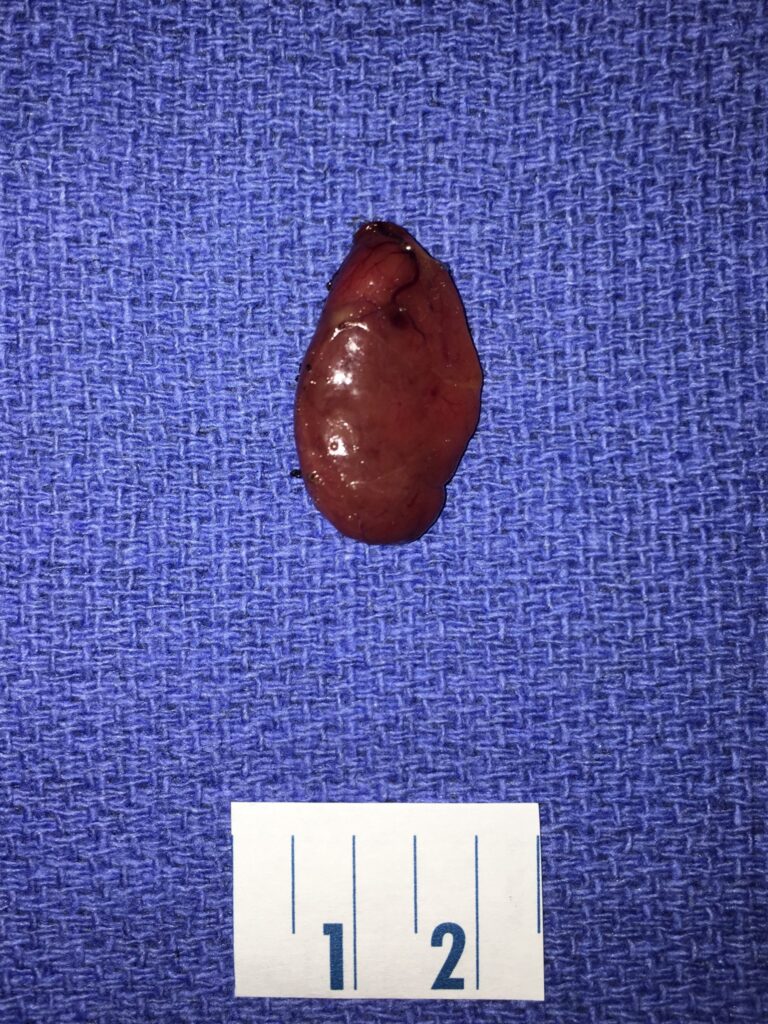
This is a picture of a typical appearing parathyroid adenoma. The ruler beneath the adenoma is 2.5 cm in length (the size of the incision). This adenoma was removed from a 33 year-old woman who did not have any symptoms, yet her calcium was very high (11.6). Because of its size, it was easily seen before surgery with both ultrasound and sestamibi scans.
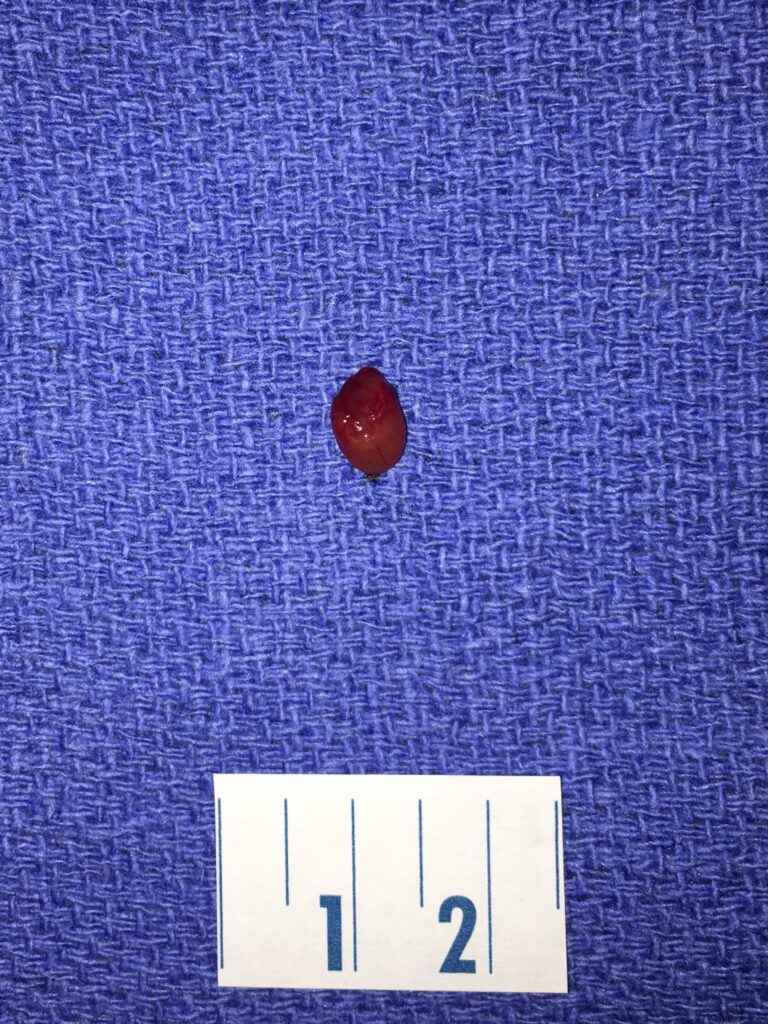
Here is a picture of a very small parathyroid adenoma. Again, the ruler is 2.5 cm in length. This adenoma was removed from a 44 year-old man who had numerous kidney stones (requiring lithotripsy on at least 5-6 occasions), bone pain, memory problems, and fatigue. His calcium level before surgery was only 10.6, despite the severity of his symptoms. Since his adenoma was so small, it didn’t show up on any scans before surgery.
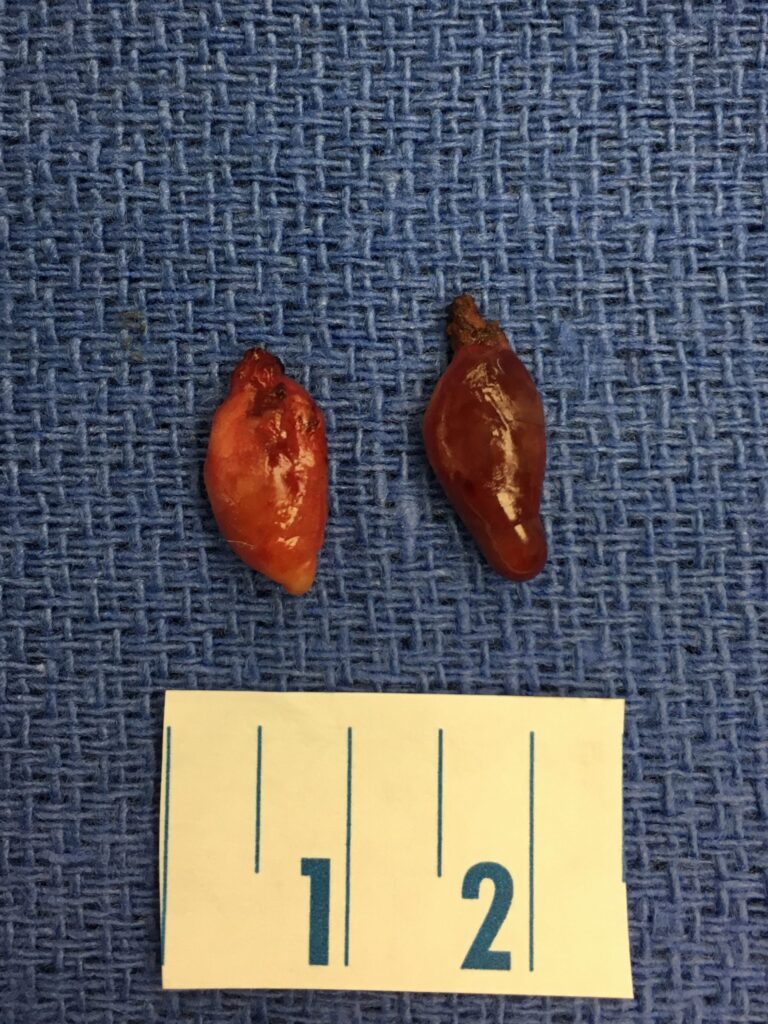
About 15% of the time, there is not one but two abnormal parathyroid glands. Often times, the larger of the two will show up on scans, but the smaller one usually does not. Both need to be removed to cure the disease, and the optimal time to do so is in the initial operation. Rarely, three or even all four parathyroid glands can be overactive. All four glands can be evaluated through the same one inch incision, and any abnormal gland can be removed. Only half of one parathyroid gland is all the tissue which is necessary for normal parathyroid function and normal calcium maintenance.
Surgery is the only definitive treatment for primary hyperparathyroidism. It seems simple enough to remove the bad gland or glands, but this is a very challenging operation because of the important anatomy in this location.
On each side of the neck is a nerve (the recurrent laryngeal nerve) which activates the vocal cords. These nerves are very fragile, and if they are manipulated too much during surgery, they will be weak afterwards. If one nerve is weak and the other is functioning normally, the voice will be hoarse (sometimes even hard to talk at all). Fortunately, the nerves recover their function in most instances and the hoarseness will resolve over a period of weeks to months. If both of the nerves are weak at the same time, it becomes difficult to breathe so that a breathing tube (tracheotomy tube) may need to be placed into the neck until the nerves recover function. If the nerves are cut, their function will never recover so it is very important for a surgeon to find the nerves and be very gentle with them so that their function is not compromised.
Sometimes it is not possible to find the bad gland during surgery, but an experienced parathyroid surgeon generally have a failure rate of less than 1%. For surgeons with less experience, the number will be higher. It is also possible for a surgeon to remove too much parathyroid tissue creating a condition called hypoparathyroidism, where the body cannot make enough parathyroid hormone from all of the glands being removed or injured at the time of surgery. This is a very rare occurrence for an experienced surgeon, as even half of one normal gland can produce enough hormone to maintain normal calcium levels. Unfortunately, there is no cure for permanent hypoparathyroidism and the only treatment is taking calcium supplements multiple times per day or a very expensive synthetic parathyroid hormone medication.
Routine surgical training programs for general surgeons and ENT (ear, nose, and throat) physicians only dedicate a few weeks to this operation despite the fact that it is very difficult operation to perform successfully. An experienced surgeon has likely done an additional year of training called a fellowship in endocrine surgery (thyroid and parathyroid surgery) to improve their skills at this challenging procedure. An experienced surgeon who performs this operation regularly does not need drains, large incisions, or overnight hospitalization after the procedure. Choosing an experienced surgeon a parathyroidectomy is the most important factor in having a successful operation without complications.
For more information on thyroid and parathyroid diseases, visit www.thyroidandparathyroid.com.
