Minimally Invasive Thyroidectomy
Thyroid surgery is undertaken for three main reasons: removal of thyroid cancer or nodules with concern for cancer, benign growth of the thyroid gland(goiter), or abnormal hyperfunctioning of all (Graves’ disease) or part of the gland (toxic nodule). Modern thyroid surgery comes in two varieties, where half or the entire thyroid gland is removed.
This operation is best done by an experienced surgeon because there are very important structures near the thyroid which must be preserved and functional after the operation is performed. There are two recurrent laryngeal nerves, one on each side of the trachea, which activate the muscles responsible for motion of the vocal cords. Each nerve makes the vocal cord on the same side of the neck open and close, and this is important because the vocal cords open to allow us to breathe, but close to allow us to speak. A person who only has one functional recurrent laryngeal nerve has a hoarse voice, and a person without either vocal cord working may speak without difficulty, but cannot breathe well. Sometimes, a tracheotomy (breathing tube through the neck) is necessary if both vocal cords cannot move.
There are four parathyroid glands located near the thyroid work together to regulate the body’s calcium level. They produce a hormone called parathyroid hormone (PTH) which maintains the blood calcium level by increasing intestinal absorption and mobilization from the bones. Without this important hormone, calcium and vitamin D supplementation must be taken multiple times per day to maintain the body’s calcium levels. It is common for the parathyroid glands to have decreased function after surgery, but function generally recovers within a few weeks as long as the parathyroid glands are not removed or damaged during the operation.
Thyroid surgery formerly entailed a large incision which resulted in an unsightly scar across the neck, a drain in the neck, and overnight stays in the hospital with blood calcium levels drawn every 6 hours. A better understanding of anatomy and calcium physiology combined with advances in surgical technology have allowed thyroid surgery to become an outpatient procedure without a drain in the neck or the need to be stuck with a needle to check calcium levels. The size of the incision depends on the size of the thyroid gland, and can be as small as 1.5 cm for small glands with small nodules. Less surgical dissection means less postoperative pain and faster return to work (within a week).
Thyroid nodule radiofrequency ablation (RFA) is an option for many patients with troublesome nodules that are low cancer risk. This allows destruction and shrinkage of a nodule with a small office procedure (no incisions, no surgery).
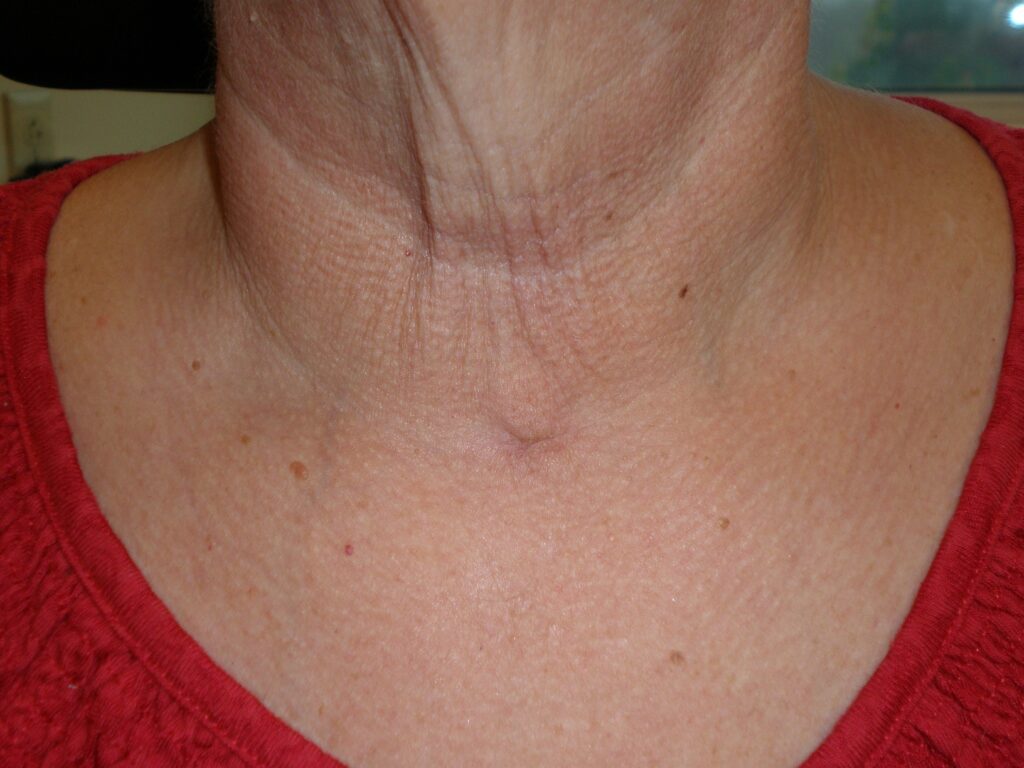
Healed Total Thyroidectomy Incision
For more information on thyroid and parathyroid diseases, visit www.thyroidandparathyroid.com.
