Snoring, Sleep-Disordered Breathing and Sleep Apnea Evaluation
Snoring is common, but it can also be a sign that airflow is partially blocked during sleep. In some patients, snoring is related to nasal congestion, enlarged soft tissues in the throat, jaw position, sleep position, or the way the airway relaxes at night. In others, snoring may occur with sleep-disordered breathing, including obstructive sleep apnea, also known as OSA.

At Advanced ENT & Allergy, our physicians evaluate the nose, throat, airway anatomy, and sleep history to help identify factors that may contribute to snoring, poor sleep quality, and disrupted nighttime breathing. The goal is to provide a practical, medically appropriate plan based on each patient’s anatomy, symptoms, sleep study results, and treatment preferences.
What Is Obstructive Sleep Apnea?
Obstructive sleep apnea occurs when the upper airway repeatedly narrows or closes during sleep. This can reduce airflow, lower oxygen levels, and interrupt normal sleep patterns. OSA can range from mild to severe and may be affected by several factors, including:
Nasal obstruction
Soft palate and throat anatomy
Tongue position
Jaw position and bite structure
Weight and neck anatomy
Sleeping on the back
Alcohol or sedating medications near bedtime
Age-related airway changes
Because OSA can involve several parts of the airway, an ENT evaluation can be helpful in identifying whether the nose, palate, tongue base, or throat structure is contributing to the problem.
Snoring vs. Sleep-Disordered Breathing
Not all snoring means sleep apnea is present. Snoring can occur when airflow causes vibration of the soft palate, uvula, tonsil area, or tongue base. However, snoring that occurs with pauses in breathing, gasping, restless sleep, or daytime fatigue may warrant additional evaluation.
A complete evaluation may include a medical history, airway examination, nasal endoscopy when appropriate, and a sleep study. Some patients may be candidates for home sleep testing, while others may need an in-lab sleep study depending on their symptoms, medical history, and insurance requirements.
Daytime Symptoms That May Be Associated With Poor Sleep Quality
Sleep-disordered breathing can affect more than nighttime rest. Common daytime concerns that may be discussed during an evaluation include:
Morning headaches
Dry mouth on waking
Daytime sleepiness
Fatigue or low energy
Difficulty concentrating
Irritability or mood changes
Waking unrefreshed
Drowsiness while reading, watching TV, or driving
High blood pressure or cardiovascular risk factors
These symptoms can have many causes, so testing and medical evaluation are important before deciding on treatment.
Jaw Position, Oral Appliances and Airway Support
The position of the lower jaw can influence the size and stability of the airway during sleep. In some patients, the airway becomes more open when the lower jaw is gently supported forward. This is the principle behind custom oral appliance therapy.
Oral appliances may be considered for selected patients with snoring or mild to moderate OSA, and for some patients who cannot tolerate CPAP. These devices are different from over-the-counter mouthguards. A properly fitted appliance is designed to support the jaw in a controlled position while helping maintain comfort and bite stability.
Positional Sleep and Snoring

For some patients, snoring and airway narrowing are worse when sleeping on the back. This is often called positional sleep-disordered breathing. In these cases, treatment may include strategies to reduce back-sleeping, improve nasal airflow, or combine positional therapy with other options.
Sleep position is only one part of the evaluation. Anatomy, nasal breathing, tongue position, weight, sleep quality, and sleep study findings all help determine the most appropriate plan.
Evaluation and Treatment Options
Advanced ENT provides evaluation and management for snoring and sleep-related breathing concerns, including:
Physician evaluation of snoring and sleep-disordered breathing
Nasal and throat airway examination
Endoscopic evaluation when appropriate
Home sleep testing and sleep study coordination
CPAP and BiPAP management
Custom oral appliance therapy
Treatment of nasal obstruction
Office-based snoring procedures when appropriate
Surgical options for selected patients
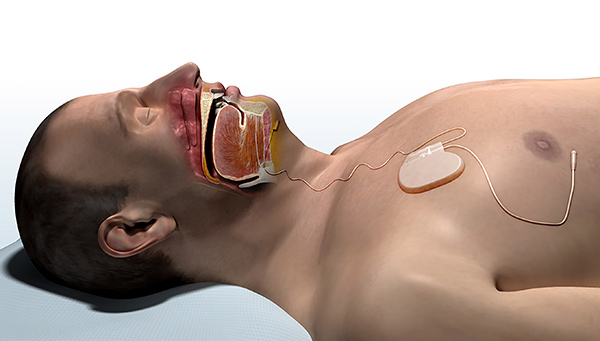
Evaluation for implantable airway stimulation therapy in appropriate candidates
Treatment recommendations are based on the type and severity of sleep-disordered breathing, airway anatomy, medical history, and patient goals. Many patients benefit from a stepwise approach that may include medical therapy, device-based treatment, office procedures, or surgery.
A Practical ENT Approach to Sleep and Breathing
Our office focuses on identifying the anatomic and medical factors that may contribute to snoring, poor sleep quality, and obstructive sleep apnea. Rather than relying on a single treatment option, we help patients understand the full range of appropriate choices, including CPAP, oral appliance therapy, nasal treatment, positional strategies, and surgical options when indicated.
